Robotic-Assisted Thymectomy
What is Myasthenia Gravis?
Myasthenia gravis (MG) is a chronic disease of the thymus gland that affects neuromuscular transmission and typically results in debilitating muscle weakness. While the thymus gland plays a key role in the disease, the exact mechanism is not fully understood.
The thymus gland is involved in the development of the immune system, which enables the body to defend itself against infection. It produces certain cells, called T-cell lymphocytes, which are a vital part of the immune system. These T-cell lymphocytes stimulate the production of antibodies whose job it is to recognize and fight off foreign invaders, called antigens, that enter the body.
Normally the antibodies destroy the antigens before major illness occurs. The basic problem that produces MG, however, involves a blockade of muscle receptors (acetylcholine) by some of these antibodies, which does harm instead of good. Damage to the receptors and impaired neuromuscular transmission ultimately leads to symptoms of MG, including weakness and fatigue.
Treatment for Myasthenia Gravis
The treatment options available to a person with myasthenia gravis depend on the severity of the condition. Some patients may not require any intervention. Others may be prescribed medications, while others may opt for surgical removal of the thymus gland. This process is called a thymectomy.
The Transcervical and Transsternal Approach
There are two widely used approaches for a thymectomy: the transcervical and the transsternal approach. The transcervical approach requires the surgeon to make an incision through the neck, while the transsternal approach involves making a long “Y” shaped incision between the chest and the breastbone. Both of these options require fairly invasive techniques.
The transsternal approach, particularly, is highly invasive. Like traditional “open heart” surgery, it involves sternotomy – cutting through the breastbone and opening the ribs. This can cause significant trauma, prolong healing time and increase the risk for serious complications and even mortality.
Robotic-Assisted Thymectomy: A Less Invasive Option
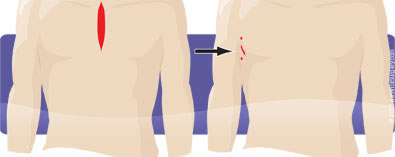 Robotic-assisted thymectomy is an alternative to the conventional transsternal approach. When performed robotically with the da Vinci Surgical System, the thymectomy is done with unparalleled precision and control through a few small incisions along the side of the chest.
Robotic-assisted thymectomy is an alternative to the conventional transsternal approach. When performed robotically with the da Vinci Surgical System, the thymectomy is done with unparalleled precision and control through a few small incisions along the side of the chest.
Benefits of Robotic-Assisted Thymectomy
In addition to avoiding the pain and trauma of sternotomy and rib spreading, this may provide patient benefits such as:
- Less risk of infection
- Less blood loss and need for blood transfusions
- Shorter hospital stay
- Significantly less pain and scarring
- Faster recovery
- Quicker return to normal activities
As with any surgery, these benefits cannot be guaranteed, as surgery is both patient- and procedure-specific. While robotic-assisted thymectomy is considered safe and effective, it may not be appropriate for every individual. Always ask your doctor about all treatment options, as well as their risks and benefits.
Illustrations courtesy of Intuitive Surgical, Inc.